loading...
A shooting incident involved2 men at Abbotsford. The Major Crime Unit takes over the investigation of the incident on Walsh near Ware. Shooting incident Just before 8 PM, officers responded to a call of possible shots being fired in the 3200 block of Walsh Avenue off Ware Road close to the Bavaria Restaurant. The officers […]
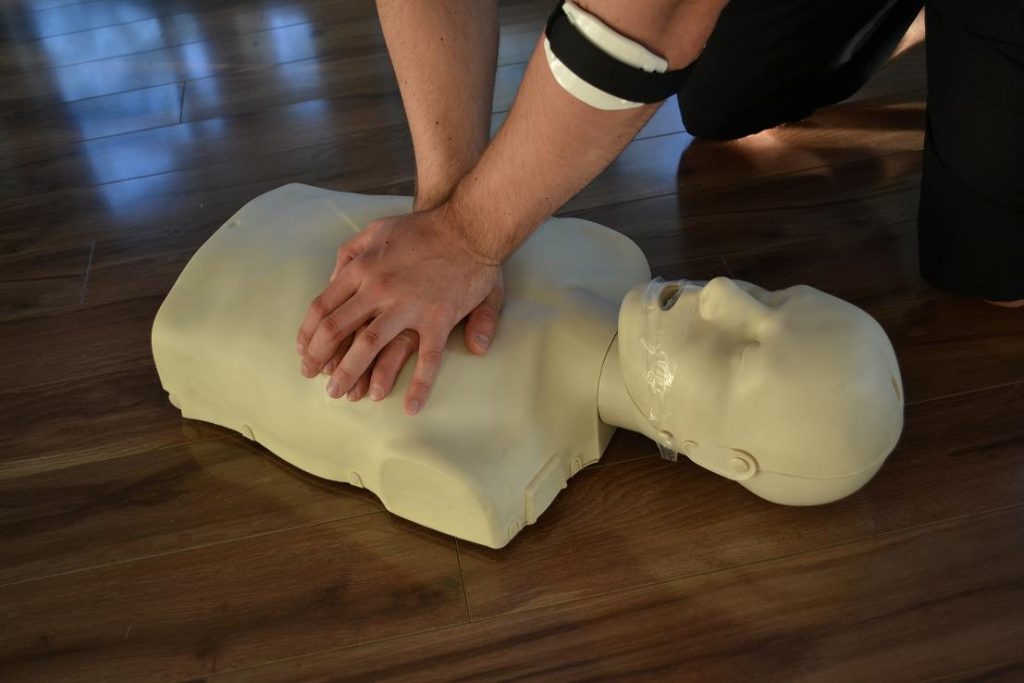
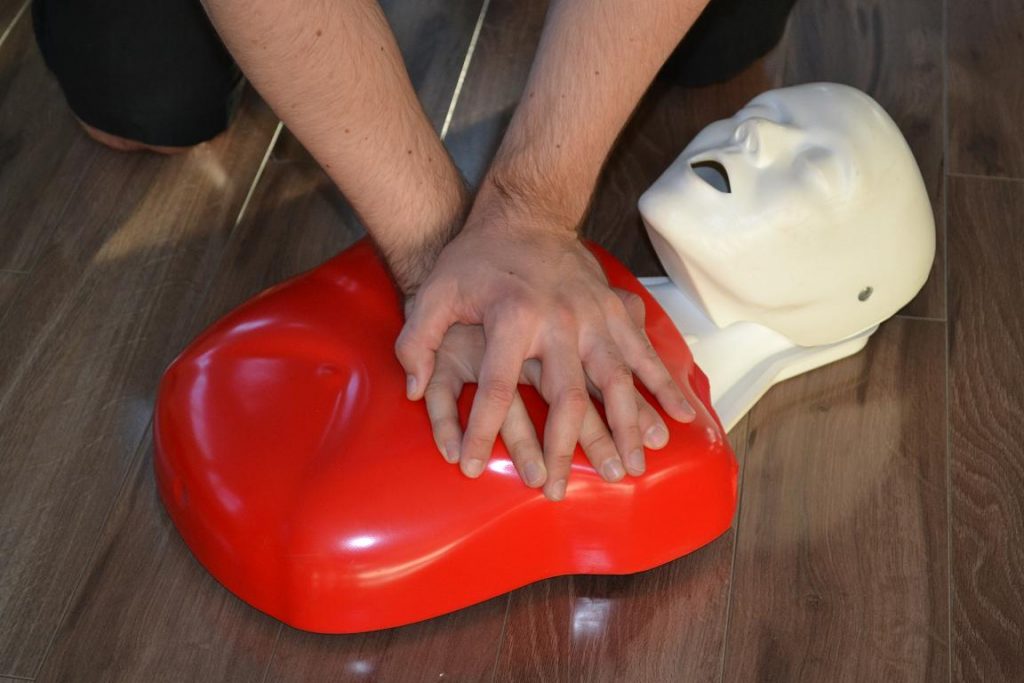
Victims of shooting ordeal receives first aid care Read More »
Two men sustained fatal gunshot wounds. Both were declared dead after a shooting incident in a small community in rural B.C. According to the police, they received a call from the community of Needles on the west shore of the Arrow Lakes after report of shots being fired. Shooting incident Based on a news release,
Victims of shooting passed away Read More »
Margaret Bell rescued a man struggling in the water. According to the firefighters, Bell went beyond when she ventured into the Glenmore Reservoir to rescue a man. The man who was struggling in the water might have gone unnoticed and drowned. For Bell, she knew what she had to do. Bell lives in the southwest
Man struggling in water given first aid care Read More »
A man was under medical distress after arriving at the border to cross from Abbotsford to the U.S. Customs and Border Protection (CBP) officers at the Huntingdon border crossing helped save the life of a 56-year old Canadian man. The Kamloops man along with his wife arrived at the border to cross from Abbotsford into
A man’s life is saved while on the border Read More »
A man is in a healthcare facility with critical injuries that require emergency care. The man was found bleeding in the parking lot of a southeast business. Unforeseen ordeal Someone called the police about a bloody man in the parking lot of a business in the 2900 block of Radcliffe Drive. The Calgary police do
A victim suffering from bleeding in critical condition Read More »
A man was recognized for helping save a drowning woman. The 23-year old Alexi Moskovski of Pierrefonds did not give much thought to the fact that he assisted in saving a drowning woman he did not know while on vacation with his parents and younger brother in Cayo Largo, Cuba. Dangers in the water Moskovski
A man recognized for saving a life Read More »
A man who was rescued by firefighters was given CPR. The man was rescued from a burning apartment suite in Vancouver. An East Vancouver apartment suite was filled with thick, black smoke when firefighters arrived and pulled a man from the building. Blazing ordeal The man was in the suite at the time. The crews
Firefighters save a life with the delivery of CPR Read More »
A mother and daughter who were thrown from their horses given CPR. A woman died after a horseback riding incident in Ladner. She was identified as 43-year old Roseanne Guerin of Ladner. Horseback riding ordeal Guerin and her 18-year old daughter were riding horses in the 3,600-block of 34th Street when the mother’s horse was
Victim of freak horse accident given CPR Read More »
A man who survived a crash a few months ago that happened at the Manitoba highway intersection is urging the officials of the province to make the area safer. Another casualty died in the same area. The man was in his early 20’s. The passenger in the other vehicle is an 18-year-old woman. She was
Man who survived crash unhappy of the latest casualty Read More »
A collision occurred at Marshall and McCallum roads. The 19-year old pedestrian died early this morning after hit by a vehicle last night in Abbotsford. The police were called around 9:40 PM to the intersection of McCallum and Marshall roads where they discovered a severely injured teen on the ground. Danger in the road According
Pedestrian given first aid road accident in Abbotsford Read More »
Serving the Vancouver Lower Mainland with the lowest priced, highest quality safety, CPR, food safe and first aid training since 2010.